Of the numerous companies disrupting primary care, one of the most interesting is Cityblock, which has deployed a model that takes care back to the neighborhood level in order to help marginalized communities. It does this by partnering with local community-based organizations to help its members get access to primary care, behavioral health care, and social services.
Of the numerous companies disrupting primary care, one of the most interesting is Cityblock, which has deployed a model that takes care back to the neighborhood level in order to help marginalized communities. It does this by partnering with local community-based organizations to help its members get access to primary care, behavioral health care, and social services.
(Vator and UCSF Health Hub are teaming up for an event in November called “Primary Care and the New Medical QB,” in which we will be talking to various stakeholders in the healthcare system, including providers, patients, and startups, about this change)
Investors have taken notice in the company, resulting the company revealing its second major funding round of 2021 on Friday: after raising a $192 million round in March, Cityblock now has another $400 million in a Series D round led by SoftBank. The new funding, which values the company at $5.7 billion, was first reported by STAT, and has since been confirmed to VatorNews.
“We can confirm that Cityblock has raised a new round of capital as we continue to accelerate our plans to empower more people across the country more quickly,” a spokesperson from Cityblock said.
Founded in 2017, Cityblock provides value-based in-home, community-based, and virtual care for Medicaid and lower-income Medicare patients.
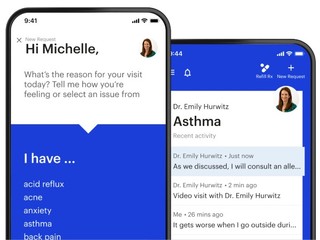
Its technology platform, called Commons, includes a communications interface, which allows care teams to text and have video chats with members. It also has an information-share and organization component, to help care teams keep track of members. In addition, Commons also provides real-time clinical decision support and evidence-based protocols.
Patients get access to a care team that includes a nurse practitioner, physician, or mental health specialist. In addition, each patient is paired with what the company calls a Community Health Partner, who acts as their care liaison, who can help the patient with coordinating transportation and filling out applications, for example.
In Cityblock’s first member cohort, the company was able to see a 15% reduction in emergency room visits and a 20% reduction in in-patient hospital stays.
Currently available in Connecticut, New York, Massachusetts, DC, and North Carolina, membership is covered by insurance and the company is currently seeing eligible EmblemHealth members in New York, ConnectiCare members in Connecticut, Tufts members in Massachusetts, and CareFirst BlueCross BlueShield members in DC.
The company says it will be using the new funding round to increase access to its services, and to bring more patients onto the platform.
“Millions of marginalized and lower income people across the U.S., including those who receive their healthcare through Medicaid plans, continue to lack sufficient access to integrated, community based health services,” the company spokesperson said.
“We are leveraging this investment to reach more people and have an even greater impact. We are focused on continuing to execute on our vision of serving 10 million members by 2030 which means scaling our operations, technology and care services.”