 While advances in healthcare technology are typically good for the patient, and the system as a whole, they are not always so great for the doctors. New techniques means more training and relearning what they already know; physician burnout has been a major problem for a while now, and this means adding even more work on top of what they already deal with.
While advances in healthcare technology are typically good for the patient, and the system as a whole, they are not always so great for the doctors. New techniques means more training and relearning what they already know; physician burnout has been a major problem for a while now, and this means adding even more work on top of what they already deal with.
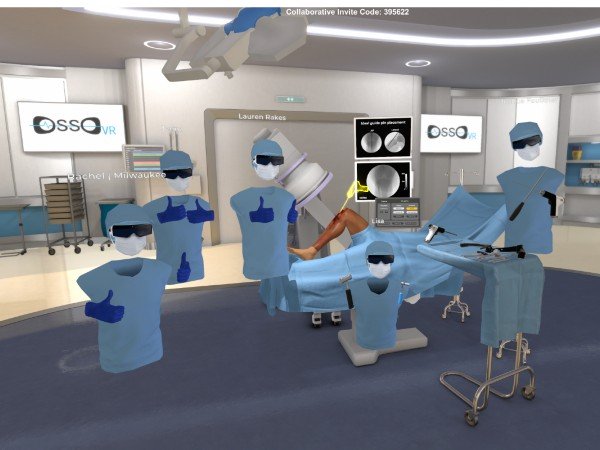
Keeping up with these advancements is an especially big problem when it comes to surgeons, where there’s already too much for them to have to learn, said Justin Barad, MD, CEO and co-founder of Osso VR, a platform that allows surgeons to practice their skills in a virtual environment.
“If you think about it, science and technology are constantly expanding the library of procedures people are expected to know how to do on demand,” he said, noting how often in the ER he would be asked to Google procedures while they were happening. In one extreme example, Barad was actually asked to operate on a gorilla at the LA Zoo, something he had no experience with.
“The reason I tell that story, other than being really cool, is that healthcare professionals deal with gorilla-like situations every day, with surgery we’ve never done before, or maybe only do very rarely, and there’s very little ability to prepare.”
In addition, all of the new technologies and techniques, like robotics, navigation, patient-specific guides and implants, and minimally invasive techniques, tend to be much harder to learn, and they’ve made modern surgery increasingly complex. That means that surgeries, which used to take 10 to 20 procedures to become proficient in, now take 50 to 100.
To solve all of this, Barad combined his medical training with his passion for gaming (he worked for Activision while he was in high school), to create Osso VR, a fully remote, VR-enabled company that allows surgeons to learn these new techniques anytime, anywhere, without the need for a lot of travel, or expensive equipment.
On Wednesday, the company announced a $27 million Series B round of funding, led by GSR Ventures, with participation from Signalfire, Kaiser Permanente Ventures, OCA Ventures, Scrum Ventures, Leslie Ventures and Anorak Ventures. This brings the company’s total funding to $43 million.
The Osso platform is used by both fully trained surgeons who are out of practice, as well as by surgeons who are early in their career, both of whom are trying to either master newer technologies or refresh themselves on procedures they perform infrequently. To use Osso, they just need a headset that they can use either in between surgeries, or at home, to perform whatever procedure they need to. Once they’re done, they get an assessment of their workflow, their ability to do steps well with clinical satisfaction, and their efficiency.
Surgeons can train by themselves, or they can do so with their team, including a surgical tech, circulating nurse, and radiology technician; they can also get coaching from experts all around the world who can give them tips and tricks.
Working with medical device manufacturers
While the medical professionals are Osso’s end users, its customers are the medical device manufacturers, including Johnson & Johnson, Stryker, and Smith & Nephew, which use the software to help train surgeons on how to use their latest equipment.
The way it usually works is that a company, such as Johnson & Johnson, will pay to fly surgeons to a place like Las Vegas, Hawaii, or Florida, where they get to experience the new technology, and practice maybe one or two times with. Allowing surgeons to train remotely saves the manufacturers both the time and money to show off their equipment in person.
“It’s not feasible to bring someone to 100 training events to master these devices. That can cost millions and millions of dollars; even a single training event might cost $250,000 and on a per surgeon basis it could be like $15,000 per attendee. So, these things are very expensive. Also, it’s hard to access, as surgeons don’t have a lot of time to travel to these things,” Barad explained.
There’s also the fact that only getting to use the equipment one or two times, and then needing to remember how to do it again a few months later, means that the surgeons are likely forget most of what was learned anyway. By partnering with these companies, Osso allows surgeons, and surgical teams, to train as much as they need to, until they reach some measured level of proficiency.
In addition, Osso also partners with healthcare institutions, including Brown University, Hospital for Special Surgery, Johns Hopkins University, and Rush University, who use the technology to train their surgeons.
Osso VR currently offers over 120 modules in over 10 specialties, and has seen nearly 30,000 training sessions completed on the platform, providing an average of 22,000 minutes of training a month. It has shown to improve surgical performance anywhere from 230 percent to 306 percent.
A growing company
Over the past year, Osso saw its engagement grown 15x year-over-year, as COVID made its platform even more of a necessity, as in-person training sessions became an impossibility during the pandemic.
“Fortunately, coming into COVID, we were a fully remote company so we were uniquely prepared to thrive under those really difficult conditions. Going through the pandemic really drove the need for this technology when in-person training was not an option at all,” said Barad.
In addition, the company, which was originally focused on orthopedics, expanded into multiple additional specialties over the last year, including orthopedics, endoscopy, and interventional procedures.
The reason, Barad explained, is that these are all surgical areas that involve more technology or imaging, making it more difficult to practice in a non-virtual setting. For example, if a surgeon wants to practice endovascular aortic aneurysm repair, they would need a patient or a cadaver, a surgical table, a facility, I would need a mobile X ray unit, a C-arm monitor, and all the instrumentation. With Osso VR, they can do all this with just an off the shelf Oculus Quest headset.
“These are techniques that involve a lot of 3D spatial concepts, a lot of steps, a lot of equipment that you need to be able to practice, so it’s really ideal to be able to do it in VR,” he said.
“That’s why these areas, like robotics and endoscopy, these are really sweet spot areas for Osso VR. That’s why these are really great focus areas. The devices themselves incorporate a lot of highly complex medical technologies that have longer learning curves.”
Going forward, the company plans to use its new funding to continue to expand its team; before the pandemic, Osso was at around 26 team members and now it’s at about 103. It will also be investing more in its product and in collecting clinical data so that it can get better insights into the impact of its technology on patient outcomes.
The ultimate goal with Osso VR is to have all 30 million health professionals around the world using its technology, Barad said.
“Success is when every single one of them can access Osso VR to train on whatever procedure they need to, at any time, whether you’re in LA, New York, Tanzania or Ethiopia. That, to me, will be a mission accomplished.”















